Infertility causes involve a variety of factors that impact either partner. Ovulatory disorders, endometriosis, hormonal imbalances, and blocked fallopian tubes are among the common infertility causes in women. Low testosterone, a decreased sperm count, or poor sperm quality are common reasons for infertility in men.
Health and lifestyle choices may also be important. You are deemed infertile if after a year of consistent unprotected sexual activity you are unable to conceive (or six months if you are over 35). The chance of becoming infertile rises with age. Thankfully a variety of treatment options are available, such as drugs, lifestyle modifications, and assisted reproductive methods like IUI and IVF.
What is infertility?
Infertility is a reproductive system condition that prevents a pregnancy from occurring after a period of trying. It can affect women, men, or both partners, and there are many possible causes.
Infertility is a reproductive system condition that prevents a pregnancy from occurring after a period of trying. It can affect women, men, or both partners, and there are many possible causes that may require infertility treatment.
Getting pregnant involves several coordinated processes in the body. First, the brain produces reproductive hormones that regulate ovarian function and allow an egg to mature in the ovary. During ovulation, the ovary releases the egg, which is picked up by the fallopian tube.
Sperm must travel through the vagina and uterus to reach the fallopian tube, where one sperm fertilizes the egg to form an embryo. The embryo then travels to the uterus, where it implants and begins to develop.
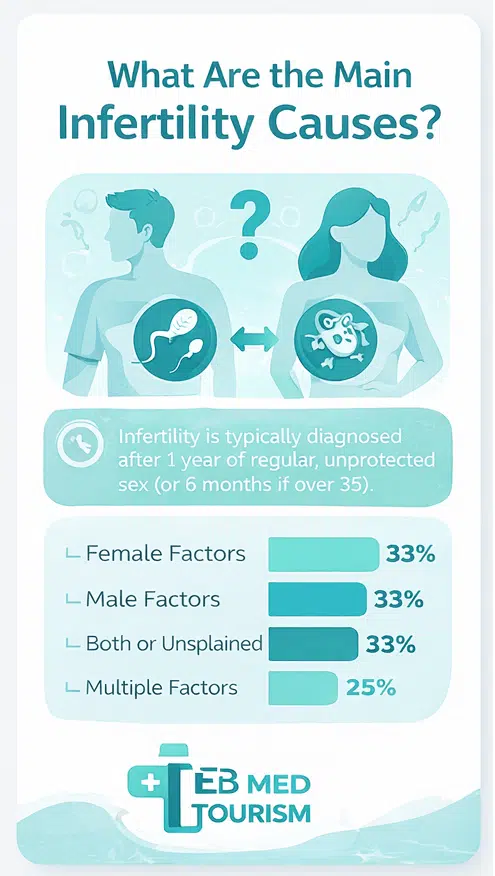
If any part of this process does not occur properly, pregnancy may not happen. Infertility is typically diagnosed after 12 months of regular, unprotected intercourse if you are under age 35, or after 6 months if you are age 35 or older. Regular unprotected sex is considered trying to conceive.
Infertility is more common than many people think. Fortunately, individuals and couples who want to start or grow a family have a wide range of treatment options available, including IVF in Iran, egg donation in Iran, sperm donation in Iran, and surrogacy in Iran.
Types of infertility
Infertility is generally classified based on a person’s reproductive history and the underlying cause. Types of human infertility include the following:
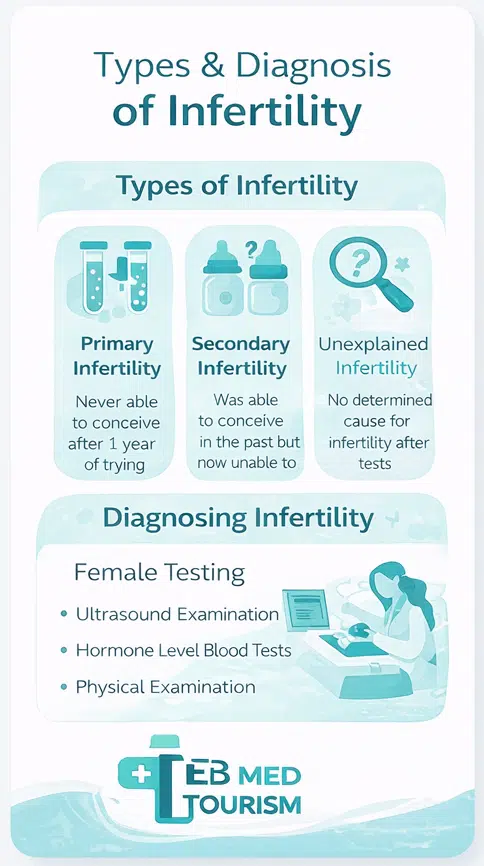
Primary infertility
Primary infertility refers to couples who have never been able to conceive after at least one year of regular, unprotected intercourse.
Secondary infertility
Secondary infertility occurs when someone has previously been pregnant but is unable to conceive again after a year of trying. In some cases, factors such as infertility after abortion may contribute.
Unexplained infertility
This type of infertility is mentioned when testing for fertility has not identified a cause for a woman’s or couple’s infertility.
What are the signs of infertility?
Failure to conceive after a year of consistent unprotected sexual activity (or six months if the woman is 35 years of age or older) is the primary sign of infertility. Nevertheless, depending on the underlying cause, some people might experience additional symptoms.
If pregnancy does not occur within the anticipated timeframe, a medical evaluation is advised because infertility can occasionally have no visible symptoms. Finding the causes and directing treatment can be aided by early assessment. However, some women or men may show physical symptoms such as:
- Pelvic or abnormal pain.
- Irregular vaginal bleeding, irregular periods, or no periods.
- Penile disorders or problems with ejaculation are often related to male infertility.
What are the infertility causes?
There are many possible infertility causes, and sometimes there is no specific reason for what causes infertility. Only a healthcare provider can determine the cause and recommend treatment. However, in 25% of cases the cause cannot be determined. Lifestyle factors such as smoking and infertility are also known to be connected.
Key Information About Infertility Causes
Category | Percentage / Detail |
Female factors | 33% |
Male factors | 33% |
Both or unexplained | 33% |
Multiple factors present | 25% of couples |
In the following, we will consider some common infertility causes in men and some infertility causes
in women:
Causes of male infertility
The most common cause of male infertility involves problems with the shape, movement (motility), or amount (low sperm count) of sperm. Such issues with sperm function, production, or delivery can lead to male infertility. The other typical infertility causes in men are as follows:
Varicocele
An increase in the veins within the loose bag of skin that contains the testicles (scrotum) is called a varicocele (VAR-ih-koe-seel). The blood from the testicles that has lost oxygen is transported by these veins.
Instead of blood flowing effectively out of the scrotum, a varicocele happens when blood pools in the veins. Varicoceles typically start during adolescence and grow over time.
Despite the possibility of some pain or discomfort, they frequently have no side effects. An infertility-causing varicocele may result in low sperm production, poor testicle development, or other issues. Such issues can be treated through varicocele surgery.
Idiopathic infertility
Some previously unidentified pathological factors, such as endocrine disruption due to environmental pollution, reactive oxygen species (ROS) generation/damage to sperm DNA, or genetic and epigenetic factors, are now thought to be linked to idiopathic male infertility.
Obstructive azoospermia
When there are no sperm in the semen, it is called azoospermia. If sperm are present in a sample, it can be determined by a semen analysis. The majority of doctors will ask you to retake the test to verify the findings. Investigating the cause is the specialty of a reproductive urologist.
When the testes are producing sperm but a physical obstruction keeps them from combining with semen during ejaculation, this condition is known as azoospermia. About 40% of all cases of azoospermia are attributed to obstructive azoospermia. It may result from a birth defect, an injury, or a vasectomy.
Hormonal disorders
Issues with the brain’s reproductive hormone-producing hypothalamus and pituitary glands can impact sperm production and sexual function. Low levels of luteinizing hormone (LH), follicle-stimulating hormone (FSH), and testosterone—all necessary for sperm production—can also result from thyroid issues.
Genetic factors
Chromosome abnormalities and single gene mutations are among the genetic causes of 10–15% of severe male infertility. While assisted reproduction techniques can circumvent this protective mechanism, natural selection stops the spread of mutations that result in infertility. Thus, determining the genetic components has emerged as a best practice for managing an infertile couple.
Previous infections and inflammation
Male infertility can result from inflammation and infections in the past that harm the reproductive organs or obstruct the sperm-transporting pathways. Sexually transmitted infections (e. g. G. Scarring swelling or obstruction in the testes epididymis or vas deferens can result from chlamydia or gonorrhea mumps after puberty prostatitis or epididymitis.
Additionally, sperm motility quality and production may all be negatively impacted by inflammation. Early intervention can sometimes avoid long-term infertility issues, but serious infections can cause irreversible harm.
Causes of female infertility
The differential diagnosis for female infertility includes conditions that can affect a woman’s ability to conceive.
To ensure clarity, these conditions are grouped according to their main mechanism or the stage of reproduction that is impacted. Each of the primary causes of female infertility will be examined to find disorders that can resemble them and should be distinguished from one another.
Polycystic Ovary Syndrome
One of the main infertility causes in women and the most prevalent endocrine condition in women is polycystic ovary syndrome. Subfertility linked to polycystic ovary syndrome is treated with a variety of medications, either alone or in combination.
Although PCOS can cause irregular cycles or a lack of ovulation, it is not in and of itself a fertility issue. It is brought on by an imbalance in the hormones that control the menstrual cycle, which impairs ovulation and may make getting pregnant more challenging.
A woman’s potential pregnancy and general health may be affected, and it is a multifactorial disorder that can result in the development of diabetes and obesity, two conditions that also negatively affect fertility. But the symptoms are not the same for every woman who has it. As a result, every case needs to be evaluated differently.
Diminished Ovarian Reserve & Advanced Maternal Age
Two prevalent reasons for female infertility are advanced maternal age (AMA) and diminished ovarian reserve (DOR). In contrast to AMA (age 35 or older), which is linked to a natural decline in fertility, an increase in chromosomal abnormalities, and an increased risk of miscarriage, DOR reduces the quantity and quality of eggs in the ovaries.
When combined, they lower the likelihood of a natural conception and may make fertility treatments less successful. However, alternatives like donor eggs or assisted reproductive technologies like IVF can enhance outcomes based on the particular circumstances.
Endometriosis (especially stages 3–4)
Endometriosis can impact fertility through a variety of factors, such as distorted pelvic anatomy, adhesions, scarred fallopian tubes, inflammation of the pelvic structures, altered immune system functioning, changes in the hormonal environment of the eggs, impaired pregnancy implantation, and altered egg quality.
During the surgery, a physician may assess the degree, location, and extent of endometriosis and provide the patient with a score and classify her as having minimal (Stage 1), mild (Stage 2), moderate (Stage 3), or severe (Stage 4) endometriosis.
Women who have severe (Stage 4) endometriosis, which causes severe scarring, blocked fallopian tubes, and damaged ovaries, have the hardest time getting pregnant.
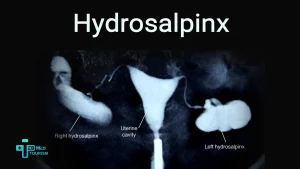
Tubal blockage or damage (hydrosalpinx, pelvic adhesions)
Because the fallopian tubes are essential for the meeting of the egg and sperm as well as the passage of the fertilized embryo to the uterus, tubal blockage or damage brought on by conditions like hydrosalpinx and pelvic adhesions is one of the main causes of female infertility.
Hydrosalpinx, which is an enlarged fallopian tube filled with fluid, and pelvic adhesions, scar tissue often caused by endometriosis infections or prior surgery, are two conditions that can partially or completely block the tubes or impair their function. This makes fertilization too difficult or increases the risk of an ectopic pregnancy and a failed implantation.
Primary Ovarian Insufficiency (POI / Premature Ovarian Failure)
One of the root infertility cause
in women is primary ovarian insufficiency (POI), commonly referred to as premature ovarian failure.
Infertility is reduced when menstrual cycles are irregular or nonexistent and the ovaries stop functioning normally before the age of 40 because the ovaries produce less estrogen and do not release eggs on a regular basis.
While some women with POI are able to conceive naturally, many do not. Low estrogen and high follicle-stimulating hormone (FSH) levels are commonly detected by hormone testing.
Uterine fibroids (especially submucosal and intracavitary)
In 2-4 percent of women, uterine fibroids may be one of the main infertility causes in women. Fibroids have been linked to infertility and recurrent pregnancy loss depending on where they are located in the uterus. The resection of submucosal fibroids has been demonstrated to increase pregnancy rates, although pregnancy and live birth rates seem to be low in these women.
Hypothalamic-pituitary hormonal disorders (hyperprolactinemia, hypogonadotropic hypogonadism)
Hyperprolactinemia and hypogonadotropic hypogonadism are examples of hypothalamic-pituitary hormonal disorders that frequently cause female infertility by interfering with the hormonal signals necessary for ovulation.
The release of GnRH, FSH, and LH is disrupted by these disorders, which results in irregular or absent ovulation, irregular menstruation, and infertility.
Unexplained female infertility
If a woman has regular ovulation and open fallopian tubes free of adhesions, fibrous growths, or endometriosis, and if the man produces normal sperm, then infertility may be considered unexplained.
The couple must have been trying to conceive for at least the last two years, and they must have had frequent sexual activity at least twice a week, especially during the period of ovulation.
Based on these standards, the most frequently cited statistics indicate that unexplained infertility affects roughly 10% of all infertile couples. However, it is believed that if careful screening is done, this number may be lower. The extent to which diagnostic tests are carried out is crucial because some studies indicate that about 28% of patients have infertility that cannot be explained.
Intrauterine adhesions (Asherman syndrome)
The development of scar tissue within your uterus is known as Asherman syndrome. Dilation and curettage (D&C) and other uterine procedures are the most common causes of it. Infertility, irregular periods, and pelvic pain can all be symptoms of Ashermans syndrome.
Asherman syndrome (AS) is a more severe and specific form of IUAs with significant scarring that may result in infertility, recurrent pregnancy loss, or severe menstrual irregularities. IUAs, on the other hand, broadly describe the formation of scar tissue within the uterus. Scar tissue removal is the primary treatment.
Congenital uterine anomalies (septate uterus, bicornuate uterus, unicornuate uterus)
Septate, bicornuate, didelphys, and unicornuate uteri are examples of congenital uterine anomalies (CUAs), which are caused by aberrant müllerian duct formation, fusion, or resorption. Other abnormalities (such as renal, skeletal, cardiac, and abdominal wall) may be linked to these abnormalities as well as cervical and vaginal abnormalities.
Symptoms of pelvic pain, irregular menarche bleeding, and repeated miscarriages or premature births are observed in some patients with CUAs. Imaging done for another indication (such as infertility symptoms associated with nonreproductive organ systems or trauma) or physical examination results (such as longitudinal vaginal septum) are used to diagnose other patients.
How to diagnose infertility?
First, your medical team or clinic tries to learn about your sexual habits prior to infertility testing. They may offer suggestions to increase your chances of becoming pregnant. Some infertile couples, however, have no apparent reason for their infertility.
Extensive testing of both the male and female partners is necessary to diagnose infertility because a variety of factors can affect conception and a woman’s capacity to carry a pregnancy. Males are either the primary cause or a contributing factor in infertility in about half of the patients who come to us for Las Vegas fertility testing.
Male infertility diagnosis
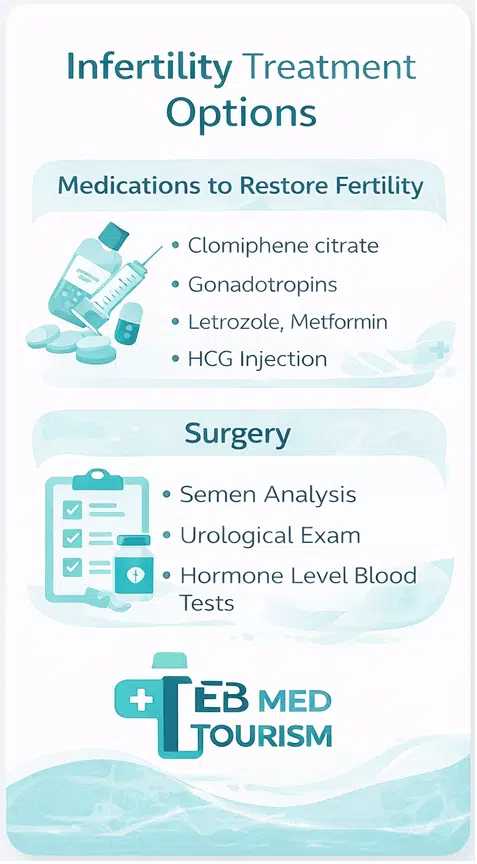
A thorough semen analysis, which can give specific details about the amount and caliber of a man’s sperm, is the initial step for men. Without treatment, getting pregnant can be challenging if there are insufficient sperm or if a significant portion of sperm are abnormally shaped or incapable of swimming. Additional male fertility tests may be required, such as a urological examination and hormone level blood tests.
Female infertility diagnosis
First-line fertility testing for women consists of a physical examination, an ultrasound examination of the reproductive organs, and hormone-level blood tests to make sure that the fallopian tubes, uterus, cervix, hormone levels, uterine lining, and ovulation patterns are all within normal limits.
In addition, each partner will give a thorough medical history that includes information about their health, sexual history, and any medical issues.
These tests, when taken together with the following, can identify a wide range of common reasons why couples are unable to conceive.
- Problems relating to sperm movement quality or quantity.
- Issues with ovulation.
- Decline in egg quality and quantity with age.
- Blockage of fallopian tubes.
- Abnormalities in the structure of the uterus.
Infertility treatment
Infertility treatment is contingent upon the cause, age, duration of infertility, and individual preferences. Due to the complexity of infertility treatment, it necessitates substantial time, financial, physical, and psychological investments. In some cases, medications such as HCG injections may be used to trigger ovulation as part of treatment.
In the following we will consider the ways for treating infertility:
Restoring fertility through medications
Fertility drugs are medications that control or promote ovulation. The primary treatment for women who are unable to conceive because of ovulation problems is fertility medication.
Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) are natural hormones that cause ovulation, and fertility medications typically function similarly. In women who ovulate, they are also used to try to stimulate a better egg or more eggs.
Fertility drugs include:
- Clomiphene citrate
- Gonadotropins
- Metformin
- Letrozole
- Bromocriptine
Surgery to restore fertility
Various surgical techniques can address issues or enhance female fertility in other ways. However, because of the effectiveness of alternative treatments, surgical procedures, such as endometriosis surgery, for fertility are becoming less common. They consist of
- Laparoscopic surgery: One minimally invasive procedure that can be used to treat infertility is laparoscopy, which involves viewing the reproductive organs (ovaries, fallopian tubes, and uterus). A system comprising a small camera and surgical instruments is used to perform this type of surgery. The surgeon will make a tiny abdominal incision to insert the camera used during the procedure.
- Hysteroscopy: In a hysteroscopy the surgeon views the uterine lining by inserting a small illuminated tube called a hysteroscope into the vagina. This procedure can be used to monitor for problems with the size and shape of the uterus and to diagnose abnormal bleeding. Polyps and small fibroids in the uterus are among the problems that can be surgically removed with it.
Conclusion
Human infertility can result from a variety of factors that affect both partners. The most common infertility causes in women are ovulatory disorders, endometriosis, uterine abnormalities, hormonal imbalances, tubal damage, and age-related decline in egg quality. Infertility in men is caused by issues with sperm production or function. New research fields like infertility and stem cells might provide treatment options in the future.
If you are seeking advanced and affordable fertility care, TebMedTourism provides you with all necessary services from the very first step with free consultation through connecting you with experienced specialists, modern clinics, and personalized treatment plans, making high-quality infertility diagnosis and treatment more accessible internationally.
What are the main causes of being infertile?
Infertility can come from many factors affecting either partner. The main causes of infertility in women include ovulation issues, hormonal imbalances, fallopian tube blockages, endometriosis, and age-related egg decline. Infertility causes in men involve hormone problems, low sperm counts, or poor sperm quality. Of course, sometimes no clear cause is found.
What are 5 causes of infertility in females?
Five common causes are polycystic ovary syndrome (PCOS) and ovulation problems, endometriosis, blocked or damaged fallopian tubes, diminished ovarian reserve or age-related fertility decline, and hormonal disorders that affect ovulation.
What to do when infertile?
You should consult a fertility specialist if you have been trying unsuccessfully for a year (or six months if you are over 35). They can test both partners and suggest medications, lifestyle changes, surgery, or assisted reproductive technologies like IVF or IUI. Many people do become parents if they receive the proper support.
What are the causes of secondary infertility?
Causes of secondary infertility involve advanced age (over 35), which affects the number of eggs available for conception; blocked or damaged fallopian tubes, which prevent sperm from reaching an egg; and complications from a prior delivery or surgery, endometriosis, medications, and polycystic ovary syndrome (PCOS).
Who is most at risk for infertility?
Risk is higher for people over 35, those with hormonal disorders, reproductive conditions (like PCOS or endometriosis), prior pelvic infections or surgeries, or unhealthy lifestyle factors (smoking, obesity, excessive alcohol). Men with sperm problems or hormone issues are also at higher risk.
At what age does infertility begin?
Fertility gradually declines with age, especially for women starting in their early 30s, with a more noticeable drop after 35. Men can remain fertile longer, but sperm quality may also decrease with age.